- This section describes the cholera surveillance strategies in surveillance units where there is no probable or confirmed cholera outbreak to ensure the early detection of a potential outbreak.
- A surveillance unit corresponds to the lowest administrative level at which decisions are made to trigger cholera prevention and control measures, and at which surveillance findings are used to inform local public health interventions. The corresponding administrative level is country specific (e.g., Administrative level 2 or Administrative level 3).
Acute watery diarrhoea
- An illness in which:
- Acute is defined as lasting less than seven days
- Watery is defined as non-bloody liquid stools that may contain mucous
- Diarrhoea is defined as three or more loose stools within a 24-hour period.
Suspected cholera case
- In the absence of a probable or confirmed cholera outbreak, a suspected cholera case is a person aged two years or older:
- with acute watery diarrhoea and severe dehydration;
or - who died from acute watery diarrhoea with no other known cause of death.
- with acute watery diarrhoea and severe dehydration;
- Patients with severe dehydration display:
- one or more danger signs:
- lethargic or unconscious
- absent or weak pulse
- respiratory distress
or
- one or more danger signs:
- at least two of the following:
- sunken eyes
- not able to drink or drinks poorly
- skin pinch goes back very slowly
Suspected cholera outbreak
- A suspected cholera outbreak is detected when:
- Two or more suspected cholera cases
or - One suspected cholera case with a positive RDT result (RDT+)
is/are reported in the same surveillance unit within seven days.
- Two or more suspected cholera cases
Probable cholera outbreak
- A probable cholera outbreak corresponds to a situation in which, based on RDT results, there is high confidence that a cholera outbreak is occurring.
- Detecting a probable outbreak through RDTs – without waiting for laboratory confirmation – allows for the rapid implementation of cholera response measures to contain the outbreak before it becomes widespread.
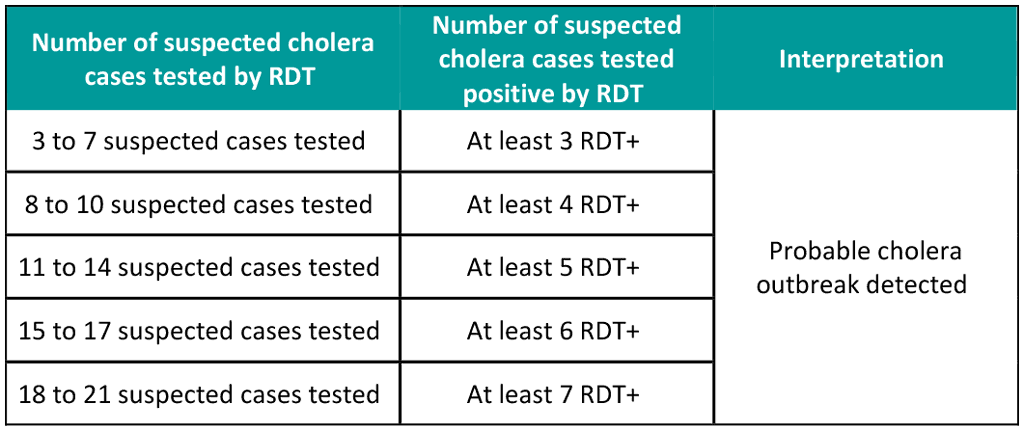
- A probable cholera outbreak is detected when the number of suspected cholera cases with a positive rapid diagnostic test (RDT+) result in the past 14 days achieves or surpasses a defined threshold, while taking into account the number of suspected cases tested (see Table 1).
Table 1. Detection of a probable cholera outbreak based on RDT+ results
- In the absence of a probable or confirmed cholera outbreak, surveillance aims to rapidly detect, investigate, and respond to any potential outbreak to contain its spread.
Detection and reporting of cases
- Three complementary surveillance streams are used to detect cholera cases: health-facility based surveillance, community-based surveillance, and event-based surveillance (unstructured information such as rumours, media content, or reports from nongovernmental organizations, community members, etc.).
- Standard data is collected on all suspected cholera cases detected in health facilities and community settings. See Appendix 2 for a template cholera case report form, Appendix 3 for a template cholera line list and Appendix 4 for a community-based surveillance template reporting form.
- Standard data on suspected cholera cases is reported to health authorities within 24 hours.
- If no suspected cholera cases are detected, the absence of cases is reported on a weekly basis (i.e., zero reporting).
Testing
- Test all suspected cholera cases.
- If RDTs are available:
- Test all suspected cholera cases by RDT
and - Collect stool samples from all RDT+ patients and send them to a reference laboratory for confirmatory testing (culture/PCR) (see Section 2 – Outbreak confirmation.
- Test all suspected cholera cases by RDT
- If RDTs are unavailable:
- Collect stool samples from all suspected cholera cases and send them to a reference laboratory for microbiological confirmation (see Section 2 – Outbreak confirmation).
- Remember:
- RDTs can be used to rule out cholera but cannot be used to confirm individual cholera cases. However, results of multiple RDTs allow for the early detection of a probable cholera outbreak.
- Clinical management of cholera cases is guided by the degree of patient dehydration and does not require any test results.
- Report RDT results to the health authorities and the laboratory if the sample is being sent there. The health authorities need the RDT results to take action and adapt the response to an outbreak; the laboratory takes into consideration the field RDT results during their own testing.
Case investigation
- If a suspected or probable cholera outbreak is detected in a surveillance unit, case investigations are conducted at the onset of the outbreak.
- Health officials interview patients to classify cases by geographic origin of infection (i.e., locally acquired or imported cases) and generate hypotheses about potential exposures and risk factors.
- Case investigations focus on the five days before illness onset, and findings should be used to guide field investigations. See Appendix 5 for a template cholera case investigation form.
Timelines and objectives
- If case investigations do not conclude with confidence that all suspected cases are imported, a field investigation is initiated quickly, preferably within 24 hours.
- Field investigation is an on-site assessment of the outbreak situation that aims to identify potential source(s) of contamination and contexts of transmission, as well as risk factors for spread.
- Field investigation should be combined with an initial needs assessment, and implementation of initial control measures (see Appendix 6 for a field investigation and initial response checklist).
Investigation team
- Field investigation is conducted by a multisectoral team. Ideally, this should include a clinical specialist with experience in case management of cholera patients, an epidemiologist, a water and sanitation expert, an infection prevention and control expert, an expert in social mobilization, community engagement, and risk communication, and a laboratory technician to support and train local laboratory staff, and oversee stool collection from suspected cases.
- All members of the investigation team should be aware of the elements to investigate and the procedures to confirm or rule out an outbreak, and should adopt a multidisciplinary approach.
- The team should work quickly and report its findings – including risks and assessed needs – to decision-makers as quickly as possible in order to provide a rapid and focused response.
- Teams should carry enough supplies to collect and transport stool samples, to treat any patients present on site, to ensure basic infection prevention and control (IPC) measures in the treatment centre, and to conduct community water, sanitation, and hygiene (WaSH) investigations. Guidelines, protocols, and information, education, and communication (IEC) materials should also be taken and left in the field.
Activities
- Engage in active case finding (i.e., look for individuals who meet the applicable definition of a suspected cholera case among individuals at risk of exposure), explore possible sources of contamination, and identify risk factors and transmission pathways. If possible, test patients’ drinking water sources for faecal contamination, or if the water is reported to be chlorinated, test for free residual chlorine (FRC).
- Map the locations of homes and water sources where people have been found to have cholera to help identify areas at risk, target interventions, and monitor disease spread.
- Implement prevention and control measures for suspected or potential risk exposures. If resources permit, a case-control or KAP study may help to identify these. Do not wait to implement prevention and control measures.
Assess the risk of spread, magnitude, and potential impact of the outbreak.
- Likelihood of transmission is based on factors such as access to safe water and improved sanitation; population behaviour (including water sources used, chlorination, open defecation, handwashing); geographical, environmental and climate conditions (expected cholera season, expected weather patterns, flooding, drought); areas with high population density (slums, camps for refugees or internally displaced persons [IDPs]), and areas with high transit of people or an influx of travellers.
- Potential impact of the disease is based on factors including existing cholera preparedness, access to treatment (oral rehydration solution [ORS] and intravenous [IV] fluids), capacity of healthcare workers to provide case management, available supplies, health-seeking behaviour, malnutrition status, and population immunity, as determined by previous exposure to cholera or previous cholera vaccination.
- Identify the available resources (human and supplies) and estimate the needs based on the risk assessment.
- Communicate these estimates quickly to local and national authorities so the necessary resources can be rapidly procured and/or provided by the government or partners.
- Calculate the supplies needed based on the expected cumulative incidence rates and the population (see Appendix 7 for a district-level supply forecasting tool).
- In rural communities with low population density, the cumulative incidence rates may vary (0.1–2 %).
- In crowded places (such as urban settings and camps for internally displaced persons and refugees), the cumulative incidence rates tend to be higher (1–5 %).
- The above actions can be taken before an outbreak is confirmed or declared.
- During the field investigations include an intervention component, such as distribution of water treatment products and ORS, and deliver key messages for health education. Interventions should be prioritized for the household and neighbours of individuals with cholera.
Additional resources:
- Public Health Surveillance for Cholera – Guidance Document 2024. Global Task Force on Cholera Control. April 2024. https://www.who.int/cholera/task_force/GTFCC-Guidancecholerasurveillance.pdf?ua=1
https://www.gtfcc.org/wpcontent/uploads/2024/04/public-health-surveillance-for-cholera-guidancedocument-2024.pdf - Global Taskforce on Cholera Control. Job Aid: Rapid Diagnostic Test (RDT) for cholera detection. Revised 2024. https://www.gtfcc.org/wp-content/uploads/2022/01/gtfcc-job-aid-rapid-diagnostic-test-for-cholera-detection-en-1.pdf
- World Health Organization – Regional Office for Africa. Technical guidelines for integrated disease surveillance and response in the WHO African Region – Booklet four. 3rd ed. 2019.https://iris.who.int/bitstream/handle/10665/312364/WHO-AF-WHECPI-02.2019-eng.pdf
- World Health Organization. Early warning alert and response (EWAR) in emergencies: an operational guide. 2022. https://www.who.int/publications/i/item/9789240063587





