- Without treatment, cholera can kill up to 50 % of patients with severe disease. Timely and appropriate treatment significantly reduces the risk of death.
- Although the benchmark for cholera treatment is a CFR of less than 1 %, deaths from dehydration from cholera should not occur.
- Approximately 80 % of people infected with cholera do not develop symptoms of the disease; these individuals can still transmit the disease by shedding V. cholerae bacteria in the environment. Bacteria are present in their faeces for up to 14 days after infection.
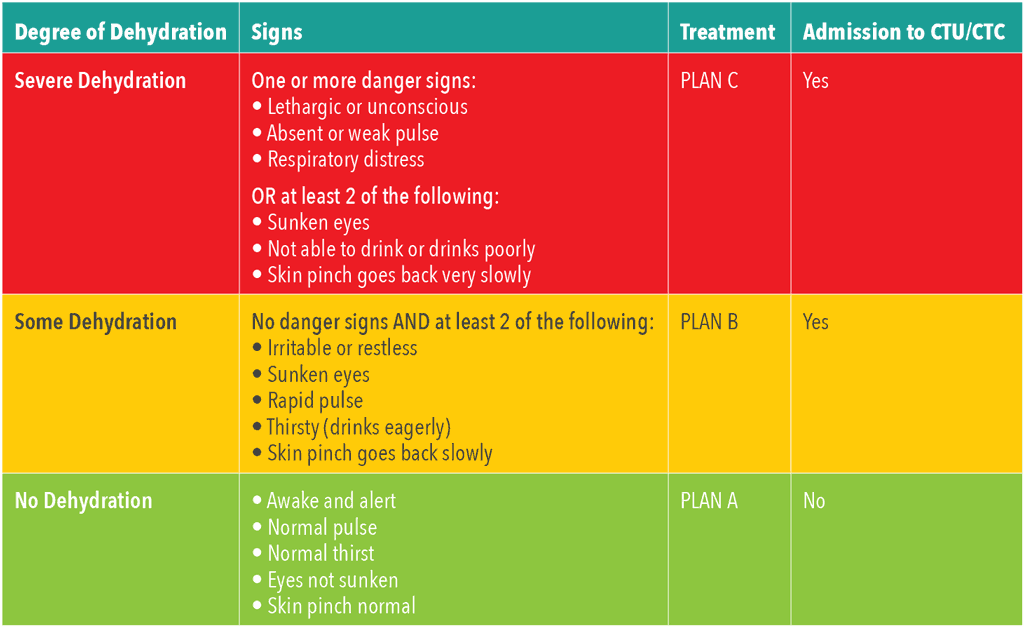
Table 3. Degree of dehydration, signs and treatment plans for cholera patients
- Among symptomatic patients, approximately 20 % will develop profuse watery diarrhoea that leads to severe dehydration and death if not treated.
- Severity of illness correlates with the number of V. cholerae bacteria ingested, lack of immunity acquired by prior exposure to the infection or vaccination, lack of breastfeeding and consequent lack of passive immunity for infants, malnutrition, immunocompromised state, reduced ability to produce gastric acid (which neutralizes the pathogen) and having blood group O.
Assessment and triage of the patient
- Assessing the degree of dehydration of the patient will determine the treatment plan (table 2).
- Severe dehydration is a medical emergency. Rapid diagnosis and treatment can save lives
- Patients with no signs or some signs of dehydration can be treated successfully by prompt administration of ORS.
- Patients with some dehydration or severe dehydration should be admitted to CTU/CTC. Patients with no dehydration can be treated at home, in the community or at an ORP.
Patient registration and admission
- Record the patient in the line list/register used at the CTU/CTC or ORP.
- For each patient, complete the admission and triage form with personal information, clinical data, physical exam and diagnosis, treatment and laboratory data (RDT results, specimens taken and sent for culture). The outcome (discharged, dead, self-discharged, referred) should be completed at later stages. See Appendix 14 – admission and triage form.
- Treatment is based on the degree of dehydration of the patient: no dehydration, some dehydration or severe dehydration. Patients with no signs or some signs of dehydration are treated with ORS (plan A and plan B, respectively). Patients with severe dehydration require IV rehydration (Plan C). See Appendix 13 – flow chart for cholera case management.
- Treatment plan A requires rehydration with ORS. It can take place at home, at an ORP or in the outpatient area at the CTU/CTC. Plan A does not require admission to the inpatient area of the CTU/CTC, however, all patients should be included in the patient line list/register.
- Treatment plans B and C require admission to the inpatient area of a CTU/CTC to correct fluid loss that has already occurred at the time of admission.
- Only patients with severe dehydration require treatment plan C, administration of IV fluids. ORS should also be given when the patient is able to drink safely.
- Antibiotics are indicated in patients with severe dehydration and, regardless of degree of dehydration, in patients with high purging (at least one stool per hour during the first 4 hours of treatment) or treatment failure (the patient is still dehydrated after completing the initial 4 hours of treatment) or in patients with coexisting conditions or comorbidities that pose elevated risk in cholera illness (see antibiotic treatment below).
- In children aged 6 months to 5 years — regardless of the degree of dehydration — zinc supplementation (20 mg p.o. zinc sulphate per day for 10 days) should be started immediately to reduce diarrhoea volume and duration.
Preparing and administering ORS
- ORS must be prepared with safe water treated with appropriate methods (see Appendix 15 – methods for household water treatment).
- ORS should be made fresh daily. It should not be stored for more than 12 hours, or 24 hours if refrigerated. Ready-made sachets containing salts and minerals are available for preparing ORS.
- ORS should be given regularly, in small amounts. If a patient vomits the ORS, slow the administration of ORS and then slowly increase again when vomiting stops.
- In addition to amounts of ORS specified in the treatment plan, patients must receive additional ORS to compensate for ongoing losses from continuing diarrhoea and vomiting.
Plan A. Oral rehydration for patients with no signs of dehydration
- Patients with no signs of dehydration should be treated with ORS.
- There is no need to admit patients with no signs of dehydration to the inpatient area of the CTU/CTC. They can be treated with ORS at home, at ORPs or at the outpatient area at the CTU/CTC.
- If the patient is seen at an ORP or CTU/CTC:
- keep the patient under observation for 2–4 hours to ensure the person is tolerating ORS; and
- during observation and before sending patients home, provide clear instructions for care. Advise the patient or caregiver to continue giving ORS after each loose stool and to come back immediately if the patient’s condition deteriorates (repeated vomiting, number of stools increased or the patient is drinking or eating poorly).
- Patients should receive ORS after each loose stool to maintain hydration until diarrhoea stops.
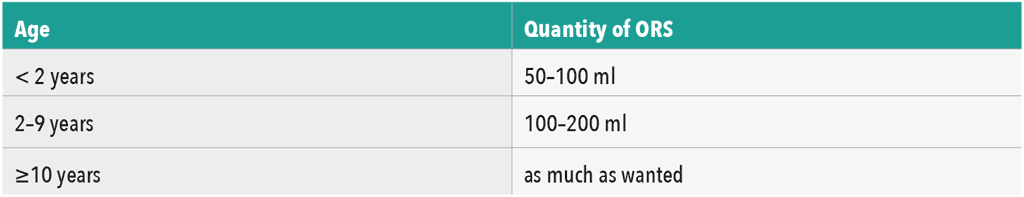
- Following each loose stool, provide the following amounts of ORS (table 3).
Plan B. Oral rehydration for patients with some dehydration
- Patients presenting with signs of some dehydration must be admitted to the CTU/CTC.
- For initial treatment, give ORS according the weight of the patient (75 ml/kg) in the first 4 hours.
- Add the specified quantity of ORS to replace on-going diarrhoeal losses (per table 3).
Table 3. Quantity of ORS to be Given after Each Loose Stool by Age Group
- Cholera patients with some signs of dehydration do not need IV fluid replacement, but they need to be monitored closely during the first 4 hours.
- If the patient has severe vomiting or is not able to drink, or if at any time signs of severe dehydration appear, then shift immediately to Treatment Plan C.
- If there are still signs of some dehydration after the first 4 hours, repeat treatment plan B for 4 hours and reassess.
- If there are no signs of dehydration after the first 4 hours of treatment, the patient can be discharged and sent home. Advise patients or caregivers to continue giving ORS after each loose stool and to come back immediately if condition deteriorates (repeated vomiting, number of stools increased or the patient is drinking or eating poorly).
Plan C. Intravenous (IV) therapy for severe dehydration
- Severe dehydration is a medical emergency and patients must be treated urgently. Seconds can make a difference.
- Patients with severe dehydration should start IV fluids immediately.
- As soon as the patient can drink, give ORS solution (per table 3) in addition to IV fluids.
- Ringer’s lactate is the first choice of IV fluid. If Ringer’s lactate is not available, the following IV solutions can be used:
- normal saline
- 5 % glucose in normal saline
- cholera saline
- Plain 5 % glucose (dextrose) solution is not recommended.
- Give a total of 100 ml/kg Ringer’s lactate solution divided in two periods. The rate of infusion in each period is slower for children younger than 1 year (see table 4).
Table 4. Quantity of Ringer’s Lactate Solution by Age Group.

- More than one IV line may be necessary to give adequate fluid during the first period (bolus treatment).
- When IV rehydration is not possible, and the patient cannot drink, ORS solution can be given by nasogastric tube. Switch to IV rehydration as soon as possible. Do not use nasogastric tubes for patients who are vomiting.
- Other systemic access such as femoral vein or intra-osseous may be used if staff are trained and necessary supplies are available.
- Patients should be encouraged to drink ORS once they are fully conscious and are not vomiting.
- Fluid output should be measured and equivalent volumes of fluid added to the amount described for initial treatment. This fluid can initially be given as IV fluid, but should be given as ORS once patients can drink safely.
- Monitor the patient closely and perform frequent reassessment (every 15–30 minutes).
- After 6 hours in children younger than 1 year or 3 hours in all other patients, perform a full reassessment. If hydration is improved and the patient can drink, switch to treatment plan B if there is still some dehydration or treatment plan A if there are no signs of dehydration.
- Children with severe acute malnutrition (SAM), elderly people and those with uncontrolled chronic conditions (such as congestive heart failure, diabetes, hypertension) are especially vulnerable to complications.
- Pulmonary oedema can occur if excessive IV fluid is given and renal failure can occur if too little fluid is given; hypoglycaemia and hypokalaemia can occur, especially in children with malnutrition who are rehydrated with Ringer’s lactate alone.
- Antibiotics can reduce the volume and duration of diarrhoea and the period of V. cholerae shedding.
- Antibiotics are indicated for:
- cholera patients hospitalized with severe dehydration
- patients with high purging (at least one stool per hour during the first 4 hours of treatment) or treatment failure (the patient is still dehydrated after completing the initial 4 hours of rehydration therapy), regardless of the degree of dehydration; and
- patients with coexisting conditions (including pregnancy) or comorbidities (such as SAM, HIV), regardless of the degree of dehydration.
- Antibiotics are given as soon as the patient is able to take oral medication (once vomiting has stopped).
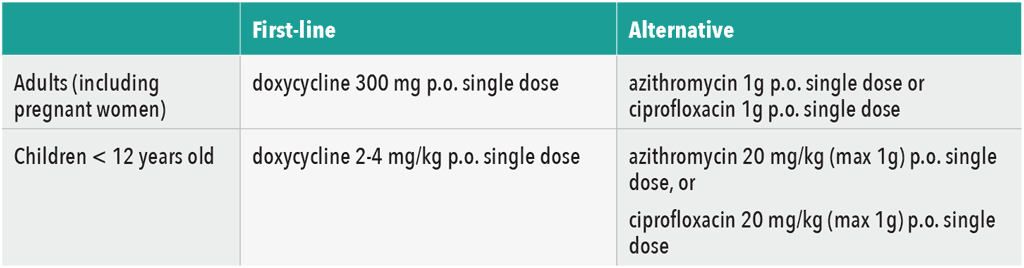
- Doxycycline — single dose (300 mg for adults; 2–4 mg/kg for children under 12 years of age) is the antibiotic of choice for all patients, including pregnant women.
- If resistance to doxycycline is documented, give azithromycin 1 g or ciprofloxacin 1 g orally as a single dose for adults. For children under 12 years of age, give azithromycin 20 mg/kg (max 1 g) or ciprofloxacin 20 mg/kg (max 1 g) orally as a single dose. See table 5.
Table 5. Antibiotic Treatment
- The laboratory should monitor patterns of resistance of the strain at the beginning of and during the outbreak and keep the clinical staff updated to adapt the treatment accordingly(see section 4 – monitoring the outbreak).
- Mass chemoprophylaxis is not recommended. Selective chemoprophylaxis can be considered in high-risk settings such as prisons.
For additional information, see GTFCC. Technical Note – Use of antibiotics for the treatment and control of cholera. May 2022
Zinc supplementation for children
- Zinc supplementation in the management of children aged 6 months to 5 years with watery diarrhoea (regardless of the cause or degree of dehydration) reduces diarrhoea volume and duration. When available, supplementation (20 mg p.o. zinc sulphate per day for 10 days) should be started immediately.
- Zinc may reduce the absorption of some classes of some antibiotics, including ciprofloxacin. For the best effect with these classes of drugs, antibiotics should be administered 2 hours before zinc or 4–6 hours after zinc.
- Children receiving therapeutic food for the treatment of SAM do not require zinc supplementation, as these foods contain sufficient zinc.
Discharge and health and hygiene education
Consider discharge if the patient:
- has no signs of dehydration
- is able to take ORS without vomiting
- has no watery stools for 4 hours
- is able to walk without assistance
- is passing urine
Prior to discharge:
- Patients should be given instructions on when to return to CTU/CTC and on how to prevent cholera.
- Provide patients and their caregivers with ORS and confirm they can correctly prepare and give ORS at home without supervision.
- Inform the patient, family members and caregivers about precautions and instructions at the household level, as follows.
- Drink and use safe water.
- Wash your hands with safe water and soap or with ABHR at critical times, including after using a toilet or handling a child’s faeces and before preparing and eating food. If caring for a patient, always wash your hands before and after providing care, after handling any soiled items (such as clothes, linens) or after touching any bodily fluids.
- Cook food thoroughly and eat it while it is still hot.
- Remove and wash any bedding or clothing that may have had contact with diarrhoeal stool with 0.2 % chlorine solution. If chlorine is not available, patients’ bedding and clothing can be disinfected by stirring for 5 minutes in boiling water and drying in direct sunlight, or by washing with soap and drying thoroughly in direct sunlight.
- If a household member develops acute, watery diarrhoea, administer ORS and seek health care immediately.
- While caring for persons who are ill with cholera, do not serve food or drink to persons who are not household members.
- Visitors may be allowed if the ill person wants company; visitors should also observe hand hygiene recommendations.
- ORS must be prepared with safe water treated with appropriate methods (see Appendix 15 – methods for household water treatment).
- ORS should be prepared daily and should not be stored for more than 12 hours at room temperature, or up to 24 hours if refrigerated
- Ready-made sachets containing salts and minerals are available for preparing ORS. The volume of clean water to be used to dissolve one sachet of ORS is marked on the sachet
Treatment of cholera in children with SAM
- Malnourished children with cholera are at risk of complications and death.
- Refer children with SAM and suspected cholera for immediate treatment at a cholera treatment facility (CTU/CTC).
- Assessment of the child’s malnutrition status and dehydration level will determine the treatment plan.
- For oral rehydration of children with SAM during an outbreak of cholera, give standard ORS. Do not give ReSoMal (Rehydration Solution for Malnutrition).
- For severe dehydration requiring IV therapy, follow rehydration guideline for malnourished children.
- Rehydration of children with SAM must be closely monitored; there is a serious risk of overhydration.
- Breastfeeding and feeding with therapeutic milk should continue throughout rehydration.
- For treatment plans in children with SAM, see
Treatment of Cholera in pregnancy
- Pregnant women with cholera are at much higher risk of losing their foetuses, compared to the general population of pregnant women. There is no evidence to show that the risk of infection or the severity of a cholera episode is higher among pregnant women.
- The risk of foetal loss depends on the degree of dehydration and vomiting, with more severe dehydration and the occurrence of vomiting increasing the risk of foetal loss.
- Antibiotic treatment should be given to all pregnant women with cholera, regardless of the degree of dehydration. See antibiotic treatment above.
- Dehydration can be difficult to assess in the later stages of pregnancy, resulting in an underestimate of the severity of dehydration. The degree of dehydration and treatment of pregnant women should be closely monitored to maintain dehydration and adequate systolic blood pressure to ensure appropriate uterine blood flow.
- The use of OCV as a preventive measure is considered to be safe and is recommended in pregnancy (see section 9 – oral cholera vaccine).
- In large outbreaks, organize the CTCs/CTUs to ensure privacy for pregnant women, especially during labour and delivery, and ensure access to reproductive health services.
Additional resources:
- Technical Note Organization of Case Management during a Cholera Outbreak. Global Task Force on Cholera Control. June 2017 https://www.who.int/cholera/task_force/GTFCC-Case-Management.pdf?ua=1
- Cholera outbreak: assessing the outbreak response and improving preparedness. Global Task Force on Cholera Control. 2010 https://www.who.int/cholera/publications/OutbreakAssessment/en/
- Managing a cholera epidemic. Chapter 5. Cholera case management. MSF. August 2017. https://medicalguidelines.msf.org/en/viewport/CHOL/english/management-of-a-cholera-epidemic-23444438.html
- Technical Note Use of antibiotics for the treatment and control of cholera. Global Task Force on Cholera Control. May 2018 https://www.who.int/cholera/task_force/use-of-antibiotics-forthetreatment-of-cholera.pdf?ua=1
- Updates on the management of severe acute malnutrition in infants and children. World Health Organization. 2013. http://www.who.int/nutrition/publications/guidelines/updates_management_SAM_infantandchildren/en/Management of severe acute malnutrition in infants and children.





